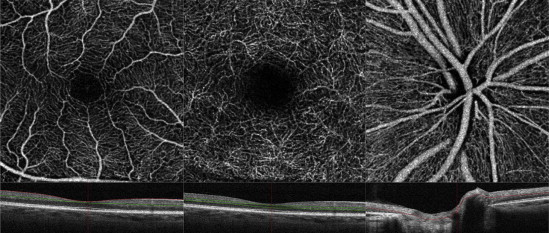
Ī recent study suggested that about 40% of diabetic patients without DR had microvascular abnormalities according to optical coherence tomographic angiography (OCTA). Since chronic hyperglycaemia can induce retinal changes even before the onset of type 2 diabetes, some studies reported that neural structural changes in the retina could be observed in patients with early-stage type 2 diabetes. The impaired neurovascular unit function can impair the ability of the retina to regulate local blood flow in response to neural activity and metabolic demands. Vascular damage can be caused by increased vascular endothelial growth factors and the production of erythropoietin and inflammatory mediators. Neurodegeneration, leading to fewer retinal ganglion cells and thinner nerve fibre layers, can be caused by increased extracellular glutamate accumulation induced excitotoxicity and reduced retinal production of neurotrophins. Hyperglycaemia and associated altered metabolic pathways can lead to neural damage (neurodegeneration),vascular damage, and impaired neurovascular unit function. Regular screening and diabetes control can help reduce the risk of developing DR. DR can be classified based on disease severity: nonproliferative DR characterised by retinal vascular abnormalities, proliferative DR characterised by retinal neovascularization, vascular abnormalities, and diabetic macular edema characterised by thickening of the retina near the macula. Risk factors of DR include long-duration diabetes, chronic hyperglycaemia, nephropathy, hypertension, and dyslipidemia. The prevalence of DR is 34.6% among adults with diabetes. 
Diabetic retinopathy (DR) is a progressive complication of diabetes in which retinal vascular damage and abnormalities can lead to vision impairment and blindness. All rights reserved.Chronic hyperglycaemia (and other factors) can trigger biochemical and physiological changes, resulting in microvascular damage and retinal dysfunction. However, those manifestations could be inconsistent according to the types of diabetes mellitus.Ĭopyright © 2020 Elsevier Inc. Our results suggested that retinal microvascular impairments might have occurred antecedent to clinically visible diabetic retinopathy and could be detected early by OCTA. In addition, subgroup analyses according to the type of diabetes mellitus indicated that most of those differences became nonsignificant (except parafoveal PD in the deep capillary plexus) in type 1 diabetes mellitus, while in type 2 diabetes mellitus they remained statistically significant. OCTA unambiguously revealed that compared with the healthy control group, the NDR group manifested enlarged areas and increased perimeters of the foveal avascular zone, with decreased perfusion density (PD) in both superficial and deep capillary plexus of the macula (except parafoveal PD of the inner retina and foveal PD) and reduced radial peripapillary capillary PD. The weighted mean differences and their 95% confidence intervals were used to assess the strength of the association.įorty-five cross-sectional studies involving 2241 diabetic and 1861 healthy eyes were ultimately included. Data of interest were extracted and analyzed by Review Manager V.5.3 and Stata V.14.0. The PubMed and Embase databases were comprehensively searched to identify studies comparing the microvascular changes between diabetic eyes without clinical retinopathy and healthy controls using OCTA. To evaluate microvascular impairments with optical coherence tomography angiography (OCTA) in the eyes of diabetic patients with no diabetic retinopathy (NDR).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
